COVID-19 & DENTISTRY
- Organization and has spread over our nation in a short time, is a highly critical public health problem.
- The transmission routes of this viral infection, which generally starts with clinical symptoms such as fever, cough and
muscle pain / weakness, are direct contact, droplet and aerosol delivery.
control strategies and additional measures for safe dental practice.

Towards the end of 2019, a pneumonia outbreak of unknown etiology occurred in Wuhan, China. The causative pathogen is called the 2019 novel coronavirus (2019-nCoV), and the disease caused by this pathogen is called 2019-coronavirus infection disease (COVID-19). The transmission rate of this virus, which can be transmitted from person to person, has increased significantly since mid-January 2020 and has spread rapidly to many countries in Europe, North America and Asia-Pacific (World Health Organization [WHO], 2020b). A global epidemic (pandemic) was declared by the World Health Organization (WHO) in the presence of 118,319 diagnosed cases and 4292 death reports in 114 countries, one day after March 10, 2020, when the first coronavirus case was reported in our country. It is known that coronavirus can be transmitted mainly by direct contact and droplet (Ge, Yang, Xia, Fu & Zhang, 2020). COVID-19 is also likely to spread when exposed to high concentrations of aerosols in a relatively closed environment. Aerosols generated during routine dental treatments pose potential risks for dentists, auxiliary staff and patients (Ge et al, 2020). Dentists; They are at risk of contracting COVID-19 due to face-to-face communication with patients, exposure to saliva, blood and other body fluids, and using sharp tools. As a matter of fact, it has been stated that dentists are more likely to be affected by the new coronavirus disease than doctors and nurses (Gamio, 2020). Dentists can also be carriers of the disease. Although there are no medically proven cases of coronavirus transmitted from the dental treatment environment, the dental treatment team should be very careful and provide a healthy environment for both patients and themselves, given the high contagiousness of the disease. In this critical process, understanding the aerosol spreading and its importance in dentistry makes it necessary to apply some special measures in addition to standard measures. The purpose of this review is to provide information about the new coronavirus epidemic, which threatens dentists closely due to their public health and occupational risk group, and to evaluate the clinic of the disease, transmission routes, necessary measures for the protection of the dentist and treatment possibilities that do not create aerosol. Aerosol Spread and Its Importance in Dentistry Droplets and Aerosols in Dental Treatment Environment When dental treatments are performed with devices with high rotational speed, the friction between the tooth and the rapidly rotating bur causes overheating in the tooth. This heat, which occurs when used without coolant, can cause irreversible pathologies in the dental pulp. For this reason, it is a universal practice to use coolant water to prevent temperature increase during routine dental procedures such as tooth cutting, decay removal, ultrasonic tooth cleaning (Farah, 2018). However; Aerosols can be formed by cooling water, ultrasonic devices, water spray, the patient's coughing, sneezing and even speech, and bio-aerosols are formed when aerosols are combined with body fluids such as blood and saliva in the oral cavity. Bioaerosols generally contain bacteria, fungi and viruses, have the potential to leach into the air for a long time, and can be inhaled by both dentists and other patients (Grenier, 1995; Jones & Brosseau, 2015). Wang et al. (Wang, Wang, Chen & Qin, 2020) studied the oral cavity of SARS patients; They detected a high rate of SARS-CoV RNA in their saliva and suggested that coronavirus transmission through oral droplets is likely. It has been proven that many cases of SARS-CoV and MERS-CoV are associated with nosocomial (hospital-acquired) transmission and result from the application of processes that generate aerosol (Chowell et al., 2015). According to the available epidemiological data, COVID-19; It has more contagiousness than SARS-CoV and MERS-CoV (Chen, 2020). For this reason, it is imperative to change the standard precautions and infection control regime by targeting COVID-19 during this epidemic.
Precautions That Can Be Taken In Dental Treatment Settings
Angiotensin converting enzyme II, the cell receptor of COVID-19 infection, is highly expressed in the oral cavity mucosa, especially in the epithelial cells of the tongue (Xu et al, 2020). These findings suggest that the oral cavity is a high-risk carrier of COVID-19 infection and prevention strategies should be considered even in a non-aerosol-producing dental / clinical setting. China National Health Commission; It has recommended that all healthcare workers use protection measures for Group A infections, a category reserved for highly contagious pathogens such as cholera and plague, for the purpose of protection from COVID-19 (Meng, Hua, Bian, 2020). In addition to the "standard measures" that can be applied in dental care settings during this epidemic, special additional measures that can be taken for aerosol spreading have been proposed in the World Health Organization's COVID-19 provisional guide and based on current clinical practices in China (WHO, 2020b). American Dental Association on March 16, 2020; recommended dentists to postpone all procedures except emergencies for the next 3 weeks (American Dental Association [ADA], 2020)
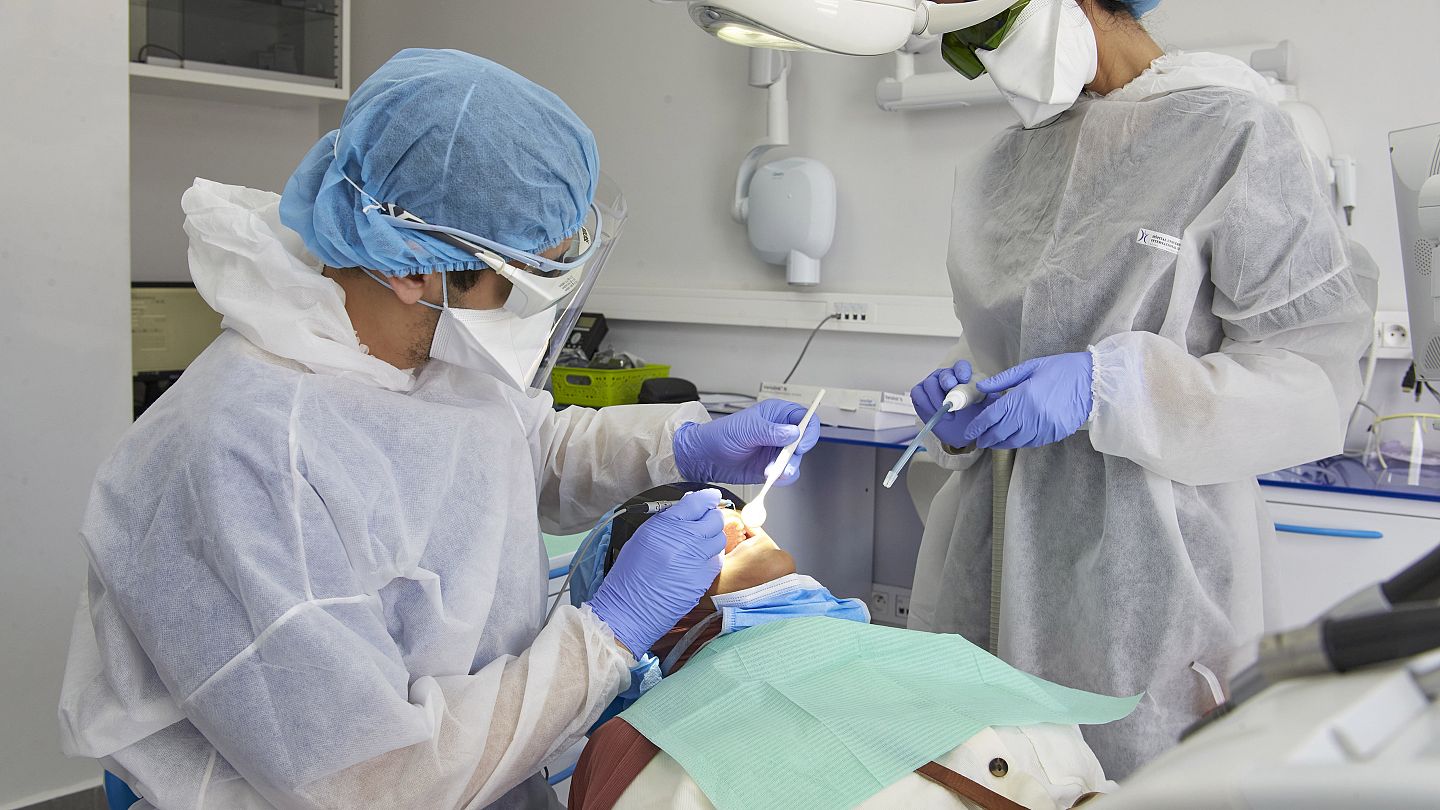
Special measures that can be applied in patient management and dental treatments
- Patient screening and triage
Planning appointments for patients with suspected / potential COVID-19 infection can be carried out by phone. Travel history including the past 14 days for the first screening, fever (37.3 C0 Should be less than), presence of respiratory tract infection symptoms such as cough, Close contact with someone diagnosed with COVID-19 and attending an event with many people situations such as should be questioned. In the event of a positive answer to one of these questions, the tooth his appointment should be postponed for at least two weeks, if possible, the patient be encouraged and report to their physicians to rule out any possibility of COVID-19. (Wang et al, 2020). Detailed medical history form, After the COVID-19 screening questionnaire and emergency survey are completed; before the examination The patient's body temperature should be measured with the non-contact method. In dental clinics, each staff member and pre-check scheme to measure and record patient's temperature as a routine procedure must be installed; Patients and accompanying persons should be allowed to enter the hospital / clinic with a medical mask. (Lai, Shih, Ko, Tang, Hsueh, 2020; Meng et al, 2020). American Disease Control and Prevention Individuals with suspected COVID-19 infection, according to central guidelines, preferably in a well-ventilated waiting area separate from other healthy individuals they must be seated. Special measures that can be applied in emergency dental treatments during the COVID-19 outbreak Dentists, strict personal protection during treatment defined as emergency must take precautions; Avoid operations that can generate droplets or aerosols, or should minimize. Four-handed studies are beneficial in controlling infection and also The use of high-volume saliva ejectors is important for the formation of droplets and aerosols. It has been reported in previous studies that it may decrease the level (Kohn et al, 2003; Samaranayake and Peiris, 2004). In addition to standard precautions during emergency dental procedures
The measures that can be taken can be listed as follows:
●As in routine, dentists should take a comprehensive medical history from each patient and He should evaluate the health status of the patient at every control appointment. During this epidemic, Screening questions for COVID-19 including personal, travel and epidemiological history should be asked. Fever and lower respiratory tract symptoms should be closely monitored. Fever and tiredness Since the symptoms may also be caused by acute dental infections, the etiology should be determined correctly. must be
● For patients with dental infections, standard emergency regimen Immediate treatments can be done following this
● Laboratory for suspected / diagnosed COVID-19 cases that are medically stable tests and multidisciplinary consultations should be requested. Patients and healthcare professionals For safety, if necessary, a new appointment should be planned for the patient after the epidemic.
● In cases with suspected or diagnosed COVID-19 infection; toothache, abscess In cases requiring emergency dental care, antibiotics and / or analgesics should be prescribed. Pharmacological treatment provides symptomatic relief as well as spreading the infection. dentistry to take all necessary precautions before dental treatments to prevent will provide some time to its employees. As an analgesic to COVID-19 infected patients, prescribing acetominophen instead of ibuprofen derivatives that suppress the immune system It has been declared necessary and this has been confirmed by the World Health Organization.
● Highest for suspected / diagnosed COVID-19 cases requiring emergency dental treatment. level of personal protection should be applied. World Health Organization; natural ventilation with at least 12 air changes per hour or at least 160 L / h per patient to facilitate recommends using a negative pressure chamber (WHO, 2020c). Without treating the next patient Mechanical ventilation should be started first.
Special precautions for routine dental treatments during the COVID-19 outbreak
Waiting area: Patient waiting areas should be adequately ventilated. Natural 60L / h is considered sufficient for each patient in ventilated rooms (WHO, 2009). There should be at least 1.8 meters of social distance between individuals. Like a sphygmomanometer or thermometer equipment, after each use, in line with the recommendations of the World Health Organization, 70% ethyl It should be disinfected using alcohol (WHO, 2016). While all patients cough and covering their nose and mouth with a handkerchief or elbows and handkerchief when sneezing
They should be informed that they should throw away the handkerchief immediately after use.
An information poster showing these basic instructions can be kept in the waiting rooms.
Hand hygiene: With the importance of hand washing in the prevention of acute respiratory infections the relevant awareness is increasing day by day. Epidemiological studies during the SARS epidemic handwashing with soap or hand rubbing with 70-90% alcohol-based disinfectants (ABEO) has been reported to prevent transmission of the disease (Rabenau, Kampf, Cinatl, Doerr,
2005).
The World Health Organization states that both hand hygiene methods are equally effective states.
If hands are visibly soiled, soap and water should be used, but If it is not visibly contaminated, alcohol-based disinfectant can be used for hand hygiene. world
Hand cleaning according to the guide published by the Health Organization; before touching a patient, Exposure to body fluids before performing any cleaning or aseptic procedure.
It should be done after staying and touching a patient (Allegranzi et al, 2007).
Disposable equipment choice: Single use to prevent cross infection It is recommended to use examination tools, caps and protective overalls (Amber Ather and Nikita, 2020). However, single-use devices will increase the total treatment costs. It is a known fact that it will cause the need for transformation.
Personal protective equipment: During dental practice, oral the spread of microorganisms towards the dentist's face and especially the infection the inner part of the eye and around the nose which is important for its spread (Bentley, Burkhart, Crawford, 1994; Nejatidanesh, Khosravi, Goroohi, Badrian, Savabi, 2013). Health at this point The equipment that the employee chooses for personal protection will be life-saving.
● Goggles and face shields: Protect the infected droplets from the human conjunctiva. COVID-19 through the mucous membrane of the eye, as it is thought to be easily contaminated. It is obvious that it can be transmitted (Lu, Liu, Jia, 2020). The aerosol and Protective glasses and / or face shield should be worn throughout the treatment to protect them from debris, These equipment should be disinfected between patient appointments or disposable shields are preferred should be.
● Face masks: In every situation working at a distance of less than 1 meter with the patient medical mask (surgical mask) should be used. In all procedures that will create aerosol (high hand tools, air-water spray and ultrasonic tartar cleaners) National Occupational Safety and Health Institute certified N95 (EU FFP2 or equivalent to European Standards) protective masks should be used. Emergency treatment in suspected COVID-19 cases During the application, higher standards such as EU FFP3 in compliance with European standards (EU149) Masks that provide protection at a degree of protection should be preferred (Ge et al, 2020). Depending on the likelihood of the spread of COVID-19 infection, personal protection Measures taken with equipment are evaluated at three different levels (Peng et al, 2020):
● Primary prevention: standard for general auxiliary staff in the clinical setting
is protection. Disposable cap, surgical mask, uniforms, gloves and protective glasses / face Includes the use of visor.
● Secondary prevention: The dentist in the clinical setting and helping him with four hands advanced protection for the physician assistant. Disposable bonnets, surgical masks, uniforms, boxes It includes the use of apron, gloves, goggles and face shield.
● Tertiary protection: suspected / diagnosed COVID-19 in a clinical setting
the dentist and the physician who helps him with four hands while caring for a patient It is the protection to be applied by his deputy. In addition to equipment in secondary protection protective overalls and shoe covers should be used. The use of double layers of gloves also reduces the risk be preferred on behalf.
The order of wearing protective equipment; in the form of gowns, masks, goggles, face shields and gloves the order of removal; should be in the form of gloves, face shield, goggles, apron and mask Using mouthwash before the procedure: Before the procedure Although its effect against coronavirus is still unknown, chlorhexidine is effective against COVID-19. mouthwash before the procedure, as this virus is sensitive to oxidation. Use of oxidative agents such as 1% Hydrogen peroxide or 0.2% Povidone has been recommended. (Peng et al, 2020).
● Rubber cover (Rubber dam) isolation: All dental aerosol producing and likely to produce Before procedures, the rubber cover application provides a barrier protection and breathing It eliminates almost all pathogens that may result from its secretion. Tire cover If correctly positioned, the only available source for contamination is the treatment the tooth will see (Harrel and Molinari, 2004). Rubber cover during cavity preparation application has been shown to reduce the spread of microorganisms by 90%. (Cochran, Miller, Sheldrake, 1989). In another study, 1 mm of rubber cover application droplets in the operation area around 70% compared to normally formed droplets. It has been reported to reduce the rate (Samaranayake, Reid, Evans, 1989). These data When evaluated accordingly, the use of rubber covers is not a choice; it is a necessity.
Contaminated air removal / filtration: Avoid contaminated air in treatment areas.
There are various methods for extracting / filtering. The most commonly used devices for this process HVE vacuum system and HEPA filters (Ge et al., 2020).
Environmental surface disinfection: Non-viable treatment of human coronaviruses such as SARS and MERS. It is known that it can stay on surfaces for up to 9 days (Kampf, Todt, Pfaender, Steinmann, 2020). However, they can be inactivated within a minute with surface disinfectants. It surface disinfectants 62-71% ethanol, 0.5% hydrogen peroxide and 0.1% (1 g / L) sodium
contains hypochlorite (Kampf et al., 2020). After each patient, especially to the operation site All surfaces roughly 2 meters away should be disinfected.
● Medical waste management: Reusable tools should be pre-treated, cleaned,
must be disinfected and stored properly. Suspected COVID-19 infection /
All medical and domestic wastes generated as a result of clinical procedures of diagnosed patients are infectious considered waste. After the waste is thrown into the medical waste bag, the mouth of the package must be connected and moved to the temporary storage area of the medical institute (Peng et al., 2020).
In addition to these measures, some strategies are included in Table 1 (Ge et al, 2020; Kariwa, Fujii, Takashima, 2006).
Aerosol-free treatments that can be applied during the COVID-19 outbreak
Without a doubt, the best treatment is to protect the tooth itself. For this purpose, tooth-borne Informing patients about infections and improving their hygiene habits. the regulation of nutritional habits and the need for further treatment. Paying attention to protective approaches is a professional precondition. However, dentine has advanced In cavitations, the dentist does not create aerosol or creates a minimal level; effective, It should be able to be applied in minimally invasive and non-invasive treatment approaches. Over the past 20 years, dental tissue has been damaged due to the complete removal of caries. Traditional treatment where the pulp tissue, which is the living part of the tooth, is weakened and damaged methods involving removal of less dental tissue and Many conservative and minimally invasive treatment approaches
(Ricketts, Kidd, Innes, Clarkson, 2008; Ricketts, Lamont, Innes, Kidd, Clarkson,
2013). Therefore, what will be the effects of the COVID-19 epidemic in our country, dentists how long patients will have to continue to delay their treatment yet for unpredictable; minimally invasive and non-invasive, which can be applied in selected cases It will be useful to know dental procedures:
Table.1. To reduce droplet formation, before and during treatment according to different science branches
applicable strategies (Ge et al, 2020, Kariwa et al, 2006)
Pre-treatment mouthwash with mouthwash
Endodontics
- Rubber dam should be applied during endodontic treatment.
- Root canal therapy is often used by many endodontic instruments and instruments. requires. Since it can be a possible source of fomite, it can be used with surfaces and equipment. unnecessary hand contact should be minimized.
Restorative and pediatric dentistry
Use of rotary instruments during cavity preparation
should be avoided. Chemomechanical caries removal in selective cases
agents or atraumatic restorative techniques can be applied.
Periodontology
Hand tools can be used to remove plaque and tartar deposits.
Prosthetic dental treatment
- Saliva ejector should be used with caution to prevent nausea reflex.
- Measuring spoons to prevent cough reflex before taking measurements
It should be chosen in appropriate sizes and adapted. In susceptible patients, the measure topical anesthesia to the throat may be considered before administration.
- During rehearsals, when the physician is contaminated with patient saliva
should not touch any items.
- Dental prosthesis, impression and bite records taken out of the patient's mouth are at least moderate. the level should be thoroughly disinfected with an effective disinfectant.
Oral, dental and maxillofacial surgery
In order not to work at the patient's breath level, simple shooting procedures
It should be done in the supine position. Suturing after tooth extraction
If necessary, a self-resorbable suture should be preferred.
Oral, dental and jaw radiology
Mouth as much as possible to avoid nausea or coughing reflex
view outside should be preferred. Oral imaging required
to prevent cross contamination, the sensor should be doubled.
must be protected with a barrier.
Chemomechanical caries removal technique
Removal of tooth decay by chemomechanical methods is one of the minimally invasive dental practices as a technique where infected dentin is softened with a chemical agent and softened dentine is removed with hand tools such as excavators. Chemomechanical caries removal technique is applied in anxious patients to remove the carious dentin in sufficient amount without using rotary tools, to protect healthy tooth tissue and at the same time to avoid pulp irritation. Both milk and permanent teeth can be applied (Ganesh & Parikh, 2011). Only to remove infected dentin, capable of remineralizing It is applied to protect dentine, which has and is less affected by bacterial invasion. techniques suggest that using rotary tools that generate aerosols are very risky. It can be preferred in pandemic and early post-pandemic conditions.
Caries covering technique Today, infected dentin can be used to prevent carious lesions. There is substantial evidence that it is not necessary to remove it completely (Dias et al, 2018; Mertz-Fairhurst, Curtis Jr, Ergle, Rueggeberg, Adair, 1998). Without removing the caries or after partial removal with hand tools, with temporary restorations on it covering the gaps and stopping its progress, temporary restoration during the epidemic physician and patient until the permanent restoration is done can provide.
Atraumatic restorative treatment
Atraumatic restorative treatment (ART) technique; removal of tooth decay with hand tools and restoring the prepared cavity with an adhesive restorative material. field is a minimally invasive technique (Van't Hof, Frencken, Helderman, Holmgren, 2006). One of the most important factors in the success of ART is that its mechanical properties are suitable and protective. It is the selection of a restorative material with property. High fluoride release in ART technique It prevents the formation of secondary caries, can bind chemically to dental tissue. Glass ionomer with high viscosity, as it is biocompatible with and oral tissues. cements are preferred (Van't Hof et al, 2006). Topical silver diamine fluoride application Silver diamine fluoride (GDF) is an effective non-invasive treatment of dental caries. agent. It does not require local anesthesia, requires minimal patient compliance and More economical than filling treatments, topical GDF application technique are its advantages. Topical GDF application, a definitive treatment in cavitation dental caries should not be considered as a method. No milk needed until permanent restorations are made. Stopping the progression of caries in permanent teeth and are prone to decay, excessive sensitivity may be observed It is recommended to be used as a preventive treatment in hypomineralized teeth. The application The subsequent black staining of the carious lesions is the most important disadvantage of GDF. Therefore, It is more preferred to use in the back areas where aesthetics are not important. Informing the family about coloration before application and obtaining consent required. Modified atraumatic restorative treatment with silver (GMART)
Gotjomonas, (1996) silver fluoride on decayed milk teeth many years ago followed by introduced this technique by applying glass ionomer restoration, then modified with silver Recently re-popularity under the name of atraumatic restorative therapy (GMART) started to win. The majority of bacteria in the cavity with GDF applied in this technique are eliminated. Thanks to the chemically bonded ART restorations, the remaining cessation of contact of bacteria with oral environment, stopping of carious lesion, remineralization and thus, it is aimed to preserve dental tissue and pulp vitality (Gotjamanos,
1996).
Hall technique
Stainless steel crowns of teeth without the need for tooth cutting and local anesthesia It is a technique in which it is restored with (PÇK). Relation of carious cavity with oral environment using Hall technique cutting and thus the bacterial content in the carious lesion changes significantly, and the progression of the carious lesion stops (Innes et al., 2017). This technique, which has proven very high levels of success in primary teeth (Innes et al. 2017), permanent molar teeth with excessive material loss, later permanent restoration or crowns It can be planned temporarily until it is done.
Post COVID-19: Future Dentistry Economic, social and psychological changes caused by the COVID-19 outbreak, in particular It will trigger a new order in many areas, including health. For dentists, dental treatment of patients other than emergency procedures during the epidemic, the current rent and personnel expenses, taxes and payable debts, re-patient care at physicians will give rise to the need. In such a case, the protection of personal health and cross Prevention of infection gaining more importance, increasing investment in these areas, will cause an increase in costs.
Use of protective equipment such as overalls, visors, goggles, masks in pediatric dentistry increased general anesthesia and sedation, as this may cause additional dental anxiety in children likely to generate demand. Dental treatments that have been delayed, it may adversely affect its quality, resulting in an increasing demand for treatment over time. Clinic Considering the disinfection requirement of the environment, after a patient treatment,
Preparing for a second patient, waiting for airing between appointments
the time required and the increased time required for a number of additional sterilization procedures a decrease in the number of patients cared for during the day. can be predicted. Increasing demands due to less patient care prolonged appointment times as a result of failure to meet and health that could not be received during the epidemic services can increase the importance and awareness of dental health. At this point, oral health and In addition to raising public awareness about dietary habits, minimally invasive
Knowing approaches, organizing dental treatment settings and possible future needs Accordingly, physicians will need to take precautions.
Conclusion
In this review, the epidemiology, symptoms, and transmission of COVID-19 infection. infection control for safe dentistry practices strategies, additional precautions and minimally invasive treatment methods, current literature evaluated in the light. During this epidemic, the conditions in which treatments can be applied, Knowing the causes and least risky treatments will shed light on dental professionals. New Since the information obtained about the coronavirus may change constantly, these measures and information It should be taken into account that the current recommendations of the national authorities must be followed.
REFERENCES
Allegranzi, B., Storr, J., Dziekan, G., Leotsakos, A., Donaldson, L., & Pittet, D. (2007). The first global patient safety challenge “clean care is safer care”: from launch to current progress and achievements1. Journal of Hospital Infection, 65 (2), 115-123. Amber Ather, B., & Nikita, B. (2020). Coronavirus Disease 19 (COVID-19): Implications for Clinical Dental Care. Journal of Endodontics, 46 (5). American Dental Association (ADA). (2020). ADA Calls Upon Dentists to Postpone Elective Procedures.https: //www.ada.org/en/press-room/news-releases/2020-archives/march/ada-callsupon-dentists-to-postpone-elective-procedures Bentley, CD, Burkhart, NW, & Crawford, JJ (1994). Evaluating spatter and aerosol contamination during dental procedures. Journal of the American Dental Association, 125 (5), 579-584. Chen, J. (2020). Pathogenicity and transmissibility of 2019-nCoV — a quick overview and comparison with other emerging viruses. Microbes and infection, 22 (2), 69-71. Chowell, G., Abdirizak, F., Lee, S., Lee, J., Jung, E., Nishiura, H., & Viboud, C. (2015). Transmission characteristics of MERS and SARS in the healthcare setting: a comparative study. BMC medicine, 13 (210), 1-12. Cochran, M. A., Miller, C. H., & Sheldrake, M. A. (1989). The efficacy of the rubber dam as a barrier to the spread of microorganisms during dental treatment. The Journal of the American Dental Association, 119 (1), 141-144. Dias, K. R., de Andrade, C. B., Wait, T., Chamon, R., Ammari, M. M., Soviero, V. M. et al. (2018). Efficacy of sealing occlusal caries with a flowable composite in primary molars: A 2- year randomized controlled clinical trial. Journal of dentistry, 74, 49-55. Farah, R. F. I. (2018). Effect of cooling water temperature on the temperature changes in pulp chamber and at handpiece head during high-speed tooth preparation. Restorative dentistry & endodontics, 44 (1). Gamio, L. (2020). The Workers Who Face the Greatest Coronavirus Risk. Obtained from https://www.nytimes.com/interactive/2020/03/15/business/economy/coronavirus-workerrisk.html Ganesh, M., & Parikh, D. (2011). Chemomechanical caries removal (CMCR) agents: Review and clinical application in primary teeth. Journal of Dentistry and Oral Hygiene, 3 (3), 34-45. Ge, Z.-y., Yang, L.-m., Xia, J.-j., Fu, X.-h., & Zhang, Y.-z. (2020). Possible aerosol transmission of COVID-19 and special precautions in dentistry. Journal of Zheijang University SCIENCE B - Biomedicine & Biotechnology, 1-8. doi: 10.1631 / jzus.B2010010 Gotjamanos, T. (1996). Pulp response in primary teeth with deep residual caries treated with silver fluoride and glass ionomer cement (atraumatic’technique). Australian Dental Journal, 41 (5), 328-334. Grenier, D. (1995). Quantitative analysis of bacterial aerosols in two different dental clinic environments. Applied and Environmental Microbiology, 61 (8), 3165-3168. Harrel, S. K., & Molinari, J. (2004). Aerosols and splatter in dentistry: a brief review of the literature and infection control implications. The Journal of the American Dental Association, 135 (4), 429-437. Centers for Disease Control and Prevention (CDC). Retrieved from https://www.cdc.gov/hai/pdfs/ppe/ppesequence.pdf. Innes, N., Evans, D., Bonifacio, C. C., Geneser, M., Hesse, D., Heimer, M. et al. (2017). The Hall Technique 10 years on: Questions and answers. British Dental Journal, 222 (6), 478-483. Jones, R. M., & Brosseau, L. M. (2015). Aerosol transmission of infectious disease. Journal of Occupational and Environmental Medicine, 57 (5), 501-508. Kampf, G., Todt, D., Pfaender, S., & Steinmann, E. (2020). Persistence of coronaviruses on inanimate surfaces and its inactivation with biocidal agents. Journal of Hospital Infection, 104 (3), 246-251. Kariwa, H., Fujii, N., & Takashima, I. (2006). Inactivation of SARS coronavirus by means of povidoneiodine, physical conditions and chemical reagents. Dermatology, 212 (Suppl. 1), 119-123. Kohn, W. G., Collins, A. S., Cleveland, J. L., Harte, J. A., Eklund, K. J., & Malvitz, D. M. (2003). Guidelines for infection control in dental health-care settings. Centers for Disease Control and Prevention-Morbidity and Mortality Weekly Report, 52. Lai, C.-C., Shih, T.-P., Ko, W.-C., Tang, H.-J., & Hsueh, P.-R. (2020). Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and corona virus disease-2019 (COVID-19): the epidemic and the challenges. International Journal of Antimicrobial Agents, 55 (3), 1-9. Lu, C.-w., Liu, X.-f., & Jia, Z.-f. (2020). 2019-nCoV transmission through the ocular surface must not be ignored. The Lancet, 395 (10224), e39. Meng, L., Hua, F., & Bian, Z. (2020). Coronavirus Disease 2019 (COVID-19): Emerging and Future Challenges for Dental and Oral Medicine. Journal of Dental Research, 1-7. doi: 10.1177 / 0022034520914246 Mertz-Fairhurst, E. J., Curtis Jr, J. W., Ergle, J. W., Rueggeberg, F. A., & Adair, S. M. (1998). Ultraconservative and cariostatic sealed restorations: results at year 10. The Journal of the American Dental Association, 129 (1), 55-66. Nejatidanesh, F., Khosravi, Z., Goroohi, H., Badrian, H., & Savabi, O. (2013). Risk of contamination of different areas of dentist's face during dental practices. International Journal of Preventive Medicine, 4 (5), 611-615. Peng, X., Xu, X., Li, Y., Cheng, L., Zhou, X., & Ren, B. (2020). Transmission routes of 2019-nCoV and controls in dental practice. International Journal of Oral Science, 12 (1), 1-6. Rabenau, H., Kampf, G., Cinatl, J., & Doerr, H. (2005). Efficacy of various disinfectants against SARS coronavirus. Journal of Hospital Infection, 61 (2), 107-111. Ricketts, D., Kidd, E., Innes, N. P., & Clarkson, J. E. (2008). Complete or ultraconservative removal of decayed tissue in unfilled teeth. Cochrane Database of Systematic Reviews (4).
https://doi.org/10.1002/14651858.CD003808.pub2. Ricketts, D., Lamont, T., Innes, N. P., Kidd, E., & Clarkson, J. E. (2013). Operative caries management in adults and children. Cochrane Database of Systematic Reviews (3). Ministry of Health, General Directorate of Public Hospitals Procurement Planning, Stock and Logistics Management Department, https://khgmstokyonetimidb.saglik.gov.tr/TR,64706/covid--19-kisiselkoruyucu-ekipman-giyme-ve-cikarma-talimati.html. Samaranayake, L., Reid, J., & Evans, D. (1989). The efficacy of rubber dam isolation in reducing atmospheric bacterial contamination. ASDC Journal of Dentistry for Children, 56 (6), 442-444. Samaranayake, L. P., & Peiris, M. (2004). Severe acute respiratory syndrome and dentistry: a retrospective view. The Journal of the American Dental Association, 135 (9), 1292-1302. Van't Hof, M. A., Frencken, J. E., Helderman, W. H. v. P., & Holmgren, C. J. (2006). The atraumatic restorative treatment (ART) approach for managing dental caries: a meta ‐ analysis. International Dental Journal, 56 (6), 345-351. Wang, Y., Wang, Y., Chen, Y., & Qin, Q. (2020). Unique epidemiological and clinical features of the emerging 2019 novel coronavirus pneumonia (COVID ‐ 19) implicate special control measures. Journal of Medical Virology, 1-9. WHO. (2009). Natural ventilation for infection control in health-care settings. From https://www.ncbi.nlm.nih.gov/books/NBK143284/pdf/Bookshelf_NBK143284.pdf
was obtained. WHO. (2016). Decontamination and reprocessing of medical devices for health-care facilities. https://apps.who.int/iris/bitstream/handle/10665/250232/9789241549851-eng.pdf?sequence=1
Obtained from. WHO. (2020a). Coronavirus disease 2019 (COVID-19): Situation Report - 59. https://reliefweb.int/report/world/coronavirus-disease-2019-covid-19-situation-report-59-19- Retrieved from march-2020. WHO. (2020b). Infection prevention and control during health care when novel coronavirus (nCoV) infection is: mail, interim guidance. Retrieved from https://www.who.int/publications-detail/infectionprevention-and-control-during-health-care-when-novel-coronavirus-(ncov)-infection-issuspected-20200125.
WHO. (2020c). Clinical Management of Severe Acute Respiratory Infection when Novel Coronavirus (2019-nCoV Infection is Suspected: Interim Guidance.). https://www.who.int/publications-detail/clinical-management-of-severe-acute-respiratory-infection-when-novel-coronavirus- Obtained from (ncov) -infection-is-mail address. Xu, H., Zhong, L., Deng, J., Peng, J., Dan, H., Zeng, X., et al. (2020). High expression of ACE2 receptor of 2019-nCoV on the epithelial cells of oral mucosa. International Journal of Oral Science, 12 (1), 1-5.

